Дотоод шүүрлийн тогтолцоо нь бидний бүх үйлдэл болон бодол мэдрэмжийг удирдаж байдаг бөгөөд эргээд бие махбодийн эрч хүч, тэжээлийн хэрэгцээ дотоод шүүрлийн идэвхжлийг тодорхойлж байдаг. Дотоод шүүрлийн идэвхжил болон эрхтэн тогтолцоонуудын нягт харилцаа холбоо нь эрүүл оршин тогтнох эх суурь болдог.
Дотоод шүүрлийн тогтолцооны гүйцэтгэх үүрэг
Дотоод шүүрлийн тогтолцоо нь үндсэн найман булчирхайт эрхтэнээс бүрддэг. Булчирхай бүр өөрийн шүүрэл ялгаруулна. Булчирхай нь шаардагдах бодисыг цуснаас сонгон шүүж авч дахин боловсруулан өөр хэлбэрт шилжүүлэн бусад эд эсэд шаардагдах химийн бодисуудыг бий болгоно. Дотоод шүүрлийн тогтолцоо нь бараг бүх эд эс, эрхтэнд нөлөөлж байдаг.
Бие биедээ харилцан дохио дамжуулах булчирхайнуудын үйл ажиллагааг хариу үйлдлийн тэнхлэг гэж нэрлэнэ. Жишээлбэл, тархины гипоталямус-өнчин тархи-бөөрний дайвар булчирхайн тэнхлэг нь гипоталямус, өнчин тархи, бөөрний булчирхай эрхтэнүүд харилцан нэг нэгнийхээ шүүрлийн хэмжээнд нөлөөлнө.
Дотоод шүүрлийн тогтолцоо нь мэдрэлийн тогтолцооны адил биеийн бүх хэсэгт дохио хүргэдэг ч дохио хүргэх хурд нь арай удаан, хэдэн цаг болон өдөр байдаг.
Булчирхайн эдээс шүүрсэн даавар цусаар дамжин зорьсон эд эрхтэнд хүрэхэд тухайн эрхтэн ямар нэг хэмжээгээр хариу үйлддэг. Дааврын хамгийн чухал үүргүүдийн нэг нь эрхтэн тогтолцоонуудын үйл ажиллагааг хооронд нь харилцан уялдуулах үүрэг юм. Жишээлбэл, зугатах шаардлага гарахад епинефрин даавар ялгарснаас зүрхний цохилт хурдсан, цусны судас тэлэгдэн булчинд хүргэх цусны хэмжээ нэмэгдэн, ходоод гэдсэнд хүрэх цусны урсгалыг багасгадаг.
Даавар нь бие махбодийн өсөлт, бодисын солилцооны хурд болон хэлбэрийг зохицуулж биеийн дотоод орчныг хэвийн хэмжээнд хадгалахад тусалдаг.
Дотоод шүүрлийн булчирхайн эрхтнүүд цусны судсаар баялаг бөгөөд ихэвчлэн шүүрэл ялгаруулах цоргогүй байдаг. Булчирхайн эс хоорондын зайны цэврүүнд даавар хуримтлуулдаг. Гадаад шүүрлийн булчирхайнуудад шүлсний, хөлсний, ходоод гэдэсний булчирхайнууд ордог бөгөөд тэдгээр нь шүүрлээ хөндийт эрхтэн рүү цоргоор ялгаруулдгаараа дотоод шүүрлийн булчирхайнаас ялгаатай.
Булчирхайнуудын үйл ажиллагааг бөөр, элэг, зүрх, өндгөвч зэрэг эрхтэнүүд дэмжиж байдаг. Жишээлбэл, бөөр нь эритропойэтин, ренин зэрэг даавруудыг шүүрүүлдэг.
Дотоод шүүрлийн тогтолцооны бүтэц
Дотоод шүүрлийн систем нь нэн шаардлагатай даавруудыг цусанд ялгаруулдаг булчирхайнуудаас бүрдэнэ. Энэхүү тогтолцоог бүрдүүлдэг гол булчирхайнууд болон хэсгүүдээс дурдъя.
Бөөрний булчирхай
Бөөрний булчирхай нь бие махбодийн шингэний тэнцвэр, стресст үзүүлэх хариу үйлдэл, нөхөн үржихүйн үйл ажиллагааг зохицуулдаг биеийн хэвийн үйл ажиллагаанд маш чухал булчирхай юм. Хоёр бөөрний дээд талд тус бүр нэг бөөрний булчирхай байрлана. Бөөрний булчирхай нь 30 гаруй төрлийн стеройд даавруудыг үйлдвэрлэдэг бөгөөд эдгээр дааврууд нь биед маш олон төрлийн үйл ажиллагааг зохицуулдаг. Эпинефрин, норэпинерфин дааврууд нь стресстэй тэмцэхэд чухал шаардлагатай зүрхний хэмийн өөрчлөлт, цусны даралт, глюкозын хэмжээ зэргийг зохицуулах үүрэгтэй.
Нойр булчирхай
Нойр булчирхай нь хэвлийн хөндийн дээд ар хэсэгт, ходоодны хойно байрладаг. Нойр булчирхайн өвөрмөц бүтэцтэй эсүүд нь цусан дахь сахарын хэмжээг тогтвортой түвшинд тэнцвэржүүлдэг инсулин болон глюкагон хоёр дааврыг ялгаруулна. Инсулин нь глюкозыг задалж, энерги болгон хувиргахад оролцдог ба цусан дахь сахарын хэмжээг бууруулдаг. Цусан дахь сахарын түвшин зохих хэмжээнээс доош буурахад глюкагон даавар нь элгэнд нөөцлөгдсөн байсан сахарыг цусанд оруулан хэмжээг нь нэмэгдүүлж, цусан дахь сахарын тэнцвэрийг зохицуулдаг.
Нойр булчирхай нь сахарын солилцооны хамтаар хоол боловсруулах үйл ажиллагаанд оролцдог. Түүний гадаад шүүрлийн эсүүдийн үйл ажиллагаагаар нийлэгжих энзимүүд \ферментүүд\ нь шүүрлийн цоргоор хоол боловсруулалтанд оролцохоор нарийн гэдэс рүү ялгардаг. Эдгээр энзимүүд нь нарийн гэдсэнд уураг, өөх тос, нүүрс усыг задална. Сахар задлах болон хоол боловсруулалтанд оролцдог хосолсон үүрэг гүйцэтгэдэг нойр булчирхай нь дотоод шүүрлийн төдийгүй мөн гадаад шүүрлийн булчирхай юм.
Өнчин тархи
Өнчин тархи нь тархины суурин доор байрладаг, маш жижиг хэмжээтэй булчирхай юм. Энэ булчирхай нь “хаан булчирхай” гэж нэрлэгдэх бөгөөд бас дотоод шүүрлийн хоорондын зохицуулалт болон булчирхайнуудын шүүрлийг уг өнчин тархи удирддаг. Өнчин тархи нь даавруудын түвшингийн мэдээлэл хүлээж авч, аливаа дааврын нэмэгдэл хэрэгцээ гарвал тухайн дааврын нийлэгжлийг нэмэгдүүлэх дохио болох өөрийн даавар болон бодисыг ялгаруулна.
Өнчин тархи урд болон арын 2 хэсгээс бүрдэнэ. Урд хэсэг нь биеийн ерөнхий өсөлтийг зохицуулдаг соматотропин, бамбай булчирхайн шүүрлийг зохицуулдаг тиротропик даавар, бөөрний дайвар булчирхайн шүүрлийг сэдээгч адренокортикотропик (ACTH), өндгөвчинд өндгөн эсийн гүйцэл болон төмсгөнд эр бэлгийн эсүүдийн хөгжилд шаардагдах фолликул өдөөгч даавар болон лютеины даавруудыг, хөхний булчирхайг сүү үйлдвэрлэлийг өдөөгч пролактин зэрэг даавруудыг ялгаруулна.
Арын хэсэг булчингийн эдийн агшилтыг өдөөгч окситоцин даавар (төрөлтийн агшилтад нэн чухал) болон бөөрний үйл ажиллагааг зохицуулдаг вазопрессин зэрэг даавруудыг ялгаруулдаг.
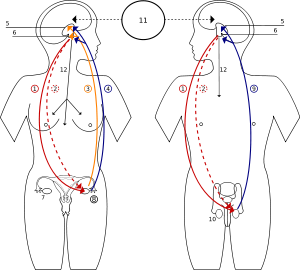
Бэлгийн булчирхай
Нөхөн үржихүйн тогтолцооны үндсэн дааврууд нь эрэгтэйчүүдийн төмсөг, эмэгтэйчүүдийн өндгөвчинд нийлэгждэг. Төмсөг нь бие махбодийн эр хүйсийн шинж тэмдэг болох булчинлаг бие галбир, баргил хоолой, сахал ургах шинж тэмдгийг хадгалах болон эр бэлгийн эсүүдийн хөгжил, эр бэлгийн дааврыг нийлэгжлийг хариуцдаг.
Эм бэлгийн дааврын нийлэгжлийг аарцгийн хөндийд байрлах хоёр өндгөвч хариуцна. Өндгөвч нь сарын тэмдгийн мөчлөг ба өндгөн эс боловсрон гүйцэхэд шаардагдах эстроген болон прогестерон даавруудыг ялгаруулна. Өндгөвчнөөс ялгарах дааврууд нь эмэгтэйлэг биеийн галбир, шингэн хоолой, хөхний хөгжил зэрэг эм хүйсийн хоёрдогч шинж тэмдгийг зохицуулдаг.
Бамбайн болон парабамбайн булчирхай
Бамбай булчирхай нь хүзүүний урд хэсэг, цээжний ясны дээд талд байрлана. Хоорондоо холбоотой хоёр хэсгээс бүрдэж мөгөөрсөн хоолойн хоёр талд байрлана. Бамбай булчирхайгаас ялгардаг дааврууд нь бие махбодийн бодисын солилцоог зохицуулна (бие махбодийн энерги үйлдвэрлэлийн химийн урвалд нөлөөлдөг).
Бамбай булчирхайн ард дөрвөн парабамбай байрлана \бамбай булчирхайн ойролцоо байрлагч\. Парабамбайн дааврууд нь цусан дахь кальцийн хэмжээг хариуцаж зохицуулна.
Дотоод шүүрэл бол биед явагддаг нэн чухал үйл ажиллагааны нэг юм. Уг тогтолцооны бүтцийг ойлгосноор, дотоод шүүрлийн өвчин эмгэгийг ойлгоход тус болно.
Дотоод шүүрлийн эмгэгүүд
Дотоод шүүрлийн тогтолцооны үйл ажиллагаа хэвийн бус болсныг цусан дахь дааврын түвшин нь хэт ихсэх эсвэл хэт буурсан байдгаар оношилдог. Булчирхайн эрхтэнүүд дааврын сэдээлтэнд хариу үйлдэл үзүүлэх чадвар алдагдсан тохиолдолд дотоод шүүрлийн эмгэгүүд үүснэ. Стресс, халдвар, цус болон бие махбодийн биологийн шингэний бүтцийн ба электролитийн тэнцвэр нь цусан дахь дааврын түвшинд нөлөөлж байдаг.
Хамгийн түгээмэл тохиолддог дотоод шүүрлийн эмгэг нь чихрийн шижин бөгөөд бие организм глюкозыг гүйцэд задалж энерги болгон ашиглаж чадахгүй байдгаас үүдэлтэй. Үндсэн шалтгаан нь глюкоз задалдаг инсулин дааврын дутагдал эсвэл, нойр булчирхай инсулиныг үйлдвэрлэсэн ч бие махбодь үр дүнтэй ашиглаж чадахгүй болсон байдаг. Үүний үр дагаварт цусан дахь сахарын хэтэрсэн хэмжээ судасны хананд тунадасжин, судасны хана болон хавь орчмын эдийг гэмтээж эхэлнэ. Харин цусан дахь сахарын хэмжээ хэт буурснаас гипоклигеми эмгэг үүснэ. Чихрийн шижингийн эмчилгээний зориулалтаар хийх инсулины тунг өндөр байлгах шаардлагатайгаас бусад тохиолдолд гипоклигеми ховор байдаг.
Нөхөн үржихүйн тогтолцооны үйл ажиллагаа дааврын тэнцвэргүй байдлаас маш эмзэг байдаг ба эмэгтэйчүүдийн эрүүл мэнд дотоод шүүрлийн үйл ажиллагаанаас хамгийн их хамаарна. Эмэгтэйчүүдийн дотоод шүүрлийн эмч нарт хандсан өвчтөнүүдийн ихэнх хувийг дотоод шүүрлийн эмгэгийн гаралтай үргүйдэл, цус алдалт, цэвэршилтийн зовиуртай эмэгтэйчүүд эзэлдэг.
Бамбайн дутагдал нь бамбай булчирхай бие махбодид хэрэгцээтэй хэмжээний бамбайн дааврыг үйлдвэрлэж чадахгүй байхыг хэлнэ. Бамбайн дааврын хомсдлын улмаас бие махбодийн үйл ажиллагаа болон солилцоо удаашрах тэр байтугай зогсох хүртэл аюултай байдаг. Бамбайн эсийн бүтэц хувиран, хяналтгүй хурдтай хуваагдсанаас бамбайн хорт хавдар үүсэн, бамбай булчирхайн дааврын хордлогын шинж тэмдгээр илрэх нь элбэг байдаг.
Аливаа дааврын түвшин ихсэх эсвэл буурснаас бие махбодийн ихэнх үйл ажиллагааны тэнцвэрт байдал алдагдана.
Даавар ясанд ч нөлөөлдөг. Ясны сийрэгжих, эсвэл яс зөөлөрч хэврэгших нь бүгд дотоод шүүрлийн зохицуулалтын гаралтай.
Та үүнийг мэдэх үү…?
Цэвэршилтийн эмгэг шинж тэмдгийн улмаас зовиурлаж байгаа эмэгтэйчүүд бамбай булчирхайн солилцооны эмгэгтэй байх магадлалтай. Цэвэршилтийн насанд ядарч сульдах, сэтгэлийн дарамттай байх, ааш араншин тогтворгүй байх, нойргүйтэх зэрэг шинж тэмдэг илрэх нь бамбайн дутагдалтай холбоотой байж мэднэ. Дотоод шүүрлийн эмч нарын хийсэн судалгаанаас харахад цэвэршилтийн шинж тэмдгийн улмаас эмчид хандсан 4 эмэгтэй тутмын нэгд нь бамбайн эмгэгийг шинж тэмдэг давхар илэрдгийг анзаарсан. Бамбай булчирхай нь бүтэн биеийн бодисын солилцоог зохицуулж, зүрх, тархи, бөөр болон нөхөн үржихүйн эрхтэн үйл ажиллагаанд чухал үүрэг гүйцэтгэхээс гадна булчингийн чадал, хоолны дуршилд ч нөлөөлдөг. Цэвэршилтийн асуудалд анхаарал хандуулахын зэрэгцээгээр насжилтын улмаас бамбайн дутагдлын эмгэг ихсэж, өвчлөлийн бусад нөхцлийг үүсгэж байгааг санах хэрэгтэй.
Цэвэршилтийн үеийн дааврын хэлбэлзэл нь таны цусан дахь сахарын солилцоог алдагдуулж болзошгүй. Цэвэршилтийн үед эм бэлгийн прогестерон даавар унахад сахарыг задалдаг инсулинд хэт мэдрэмтгий болж сахар хэт задарсан үед гэнэт бие сулрах шинж тэмдэг илрэх, харин эстроген даавар буурснаас инсулинд тэсвэртэй болж сахар задрахгүй олдмол хэлбэрээр чихрийн шижингийн шинж тэмдэг өгнө. Архаг хэлбэрийн чихрийн шижинтэй хүмүүс цэвэршилтийн насанд өвчлөлийн явц нь улам хүндрэх шалтгаан болдог. Эстроген даавар багассанаас чихрийн шижин болон зүрх судасны эмгэгтэй хүмүүсийн өвчлөлийн хүндрэх эрсдэл хамгийн өндөр байдаг. Цэвэршилтийн үеийн дотоод шүүрлийн эмгэг нь ясны сийрэгжилтийг мөн хурдасгана.
Дунд насанд дотоод шүүрлийн идэвхжил сулран биеийн жин хэт нэмэгдэн, амьдралын бололцоо сайжран хөдөлгөөний идэвхгүй болдог нь цусан дахь глюкозын хэмжээг зохицуулахад улам их хүндрэл учруулдаг.
Тиймээс шим тэжээлтэй, өөх тос багатай хоолны дэглэм барьж, шаардлагай бол кальцийн нэмэлт тэжээл хэрэглэж, хөдөлгөөний идэвхтэй байх нь маш чухал юм. Эдгээр арга хэмжээ нь холестеролын хэмжээг бууруулснаар зүрх судасны өвчин тусах эрсдлийг бууруулж, ясны сийрэгжилтээс болж яс хэврэгшихээс хамгаална.
Бэлгийн сулрал нь чихрийн шижинтэй эрэгтэйчүүдийн 35-75 хувьд нь тохиолддог түгээмэл асуудал юм. Чихрийн шижинтэй эрэгтэйчүүдийн 75 хүртэлх хувь нь амьдралынхаа хугацаанд бэлгийн сулралыг тодорхой хэмжээгээр мэдэрдэг. Чихрийн шижинтэй эрэгтэйчүүд эрүүл хүмүүстэй харьцуулахад 10-15 жилийн өмнө бэлгийн сулралд өртөж байна. Бэлгийн сулралын шалтгаан нь маш ярвигтай бөгөөд тархин дахь дотоод шүүрлийн төв стрессд дарангуйлагдах, булчингийн эд багасч, бодисын солилцоо удаашрах, зүрх судасны үйл ажиллагаа сулрах зэрэг аль ч шалтгаантай холбоотой байж болно. Үүнээс сэргийлэхийн тулд эрэгтэйчүүдийн цусны судас, мэдрэл, даавар эрүүл байх хэрэгтэйгээс гадна бэлгийн харьцааны чухлыг ухамсраар ойлгон хүндэтгэдэг байх нь чухал. Хайр ухамсар байсан ч судасны эмгэг, дааврын дутагдал, стрессийн түвшин өндөр байхад бэлгийн сулралын эмгэгт өртөж болно. Иймээс дотоод шүүрлийн үйл ажиллагааг хэвийн байлгах хувийн хариуцлагатай байж, үзлэг оношилгоо хийлгэж байх нь зүйтэй.





